Female genital mutilation/cutting
Key points
- Female genital mutilation/cutting (FGM/C) is a criminal offence in Canada.
- FGM/C is recognized as a harmful practice. It affects the physical and psychological well-being of girls and women, and has no medical benefit.
- The practice is typically performed at some point between infancy and age 15.
- Although FGM/C remains prevalent in many regions of the world, support for it varies among newcomers to Canada.
- Health care providers can help by providing a respectful and culturally informed approach to history-taking and counselling. To do this, providers need to be thoroughly aware of the medical and psychosocial consequences of this practice.
Terminology
Terms used in the medical literature include female genital mutilation/cutting (FGM/C), female genital cutting, female genital mutilation and female genital circumcision. UNICEF, the World Health Organization, the United Nations Population Fund (UNFPA) use female genital mutilation.[1][2][3] Women who have been cut, or mothers discussing the issue for their daughters, may use the terms circumcision or cutting.[4]
It is important that clinicians speak to patients using neutral and ethically sensitive language.[1][2][3]
- Clitoridectomy: Partial or total removal of the clitoris and/or the prepuce
- Infibulation: Excision of part of the external genitalia and stitching of the vulvo-vaginal opening
- Defibulation: Reopening the vulvo-vaginal opening—in a woman who has previously undergone infibulation, for sexual intercourse or childbirth
- Reinfibulation: Stitching closed the vulvo-vaginal opening or labia following defibulation
- FGM/C: All procedures involving the partial or total removal of the external genitalia, or any other injury (i.e., pricking, piercing, incising, scraping, cauterization) to the genital organs for non-medical reasons
Legal issues
FGM is internationally recognized as a violation of the human rights of girls and women. It reflects deep-rooted misogyny and suppression of female sexuality. It is usually carried out on minors and violates the rights of children.[1][2][3]
A 2021 report by the World Bank described 85 countries which have specific or general laws prohibiting FGM/C. Canada recognizes female genital mutilation (FGM) as a violation of the rights of women and girls and has criminalized its practice.[5] The Society of Obstetricians and Gynaecologists of Canada (SOGC) advises health professionals that, “reporting to appropriate child welfare protection services is mandatory when a child has recently been subjected to female genital cutting or is at risk of being subjected to the procedure.”[5] It also recommends that requests for reinfibulation be declined.
Global prevalence
An estimated 230 million girls and women worldwide have experienced FGM/C.[1] According to UNFPA, FGM is documented in 92 countries around the world[3]:
- In Africa, 33 countries generate FGM data from nationally representative data: Benin, Burkina Faso, Cameroon, Central African Republic, Chad, Cote d’Ivoire, Democratic Republic of Congo, Djibouti, Egypt, Eritrea, Ethiopia, The Gambia, Ghana, Guinea, Guinea-Bissau, Kenya, Liberia, Malawi, Mali, Mauritania, Niger, Nigeria, Senegal, Sierra Leone, Somalia, South Africa, South Sudan, Sudan, Tanzania, Togo, Uganda, Zambia and Zimbabwe.
- In the Middle East, FGM is documented in Oman, the United Arab Emirates, Yemen, Iraq, Iran, Jordan, and Palestine.
- In Asia, FGM occurs in India, Indonesia, Malaysia, Sri Lanka, Bangladesh, Thailand, Brunei, Singapore, Cambodia, Vietnam, Laos, The Philippines, Afghanistan, Pakistan, and The Maldives.
- FGM is also reported in New Zealand and Australia, Europe, North America, and South America.
There is substantial variation in prevalence within and among countries. While FGM/C is almost universal in Somalia, Guinea, and Djibouti (> 90%), it affects only 1% of girls and women in Cameroon and Uganda.[3] Higher prevalence countries tend to have less within-country variation, while lower prevalence countries tend to have more regional variation.
It is warranted to establish heightened screening for girls and young women from countries with high prevalence of FGM/C (see Figure 1). Screening girls and young women from lower-prevalence areas is also important but may be more challenging because of differing levels of support and regional variations in practice.
UNICEF reports that FGM/C is declining in some countries where it was once more common, including Sierra Leone, Ethiopia, and Burkina Faso. However, no progress has been reported in Somalia, Mali, Gambia, Guinea-Bissau, and Indonesia.[1]
Figure 1. Prevalence of FGM in countries with data (Source: UNICEF)
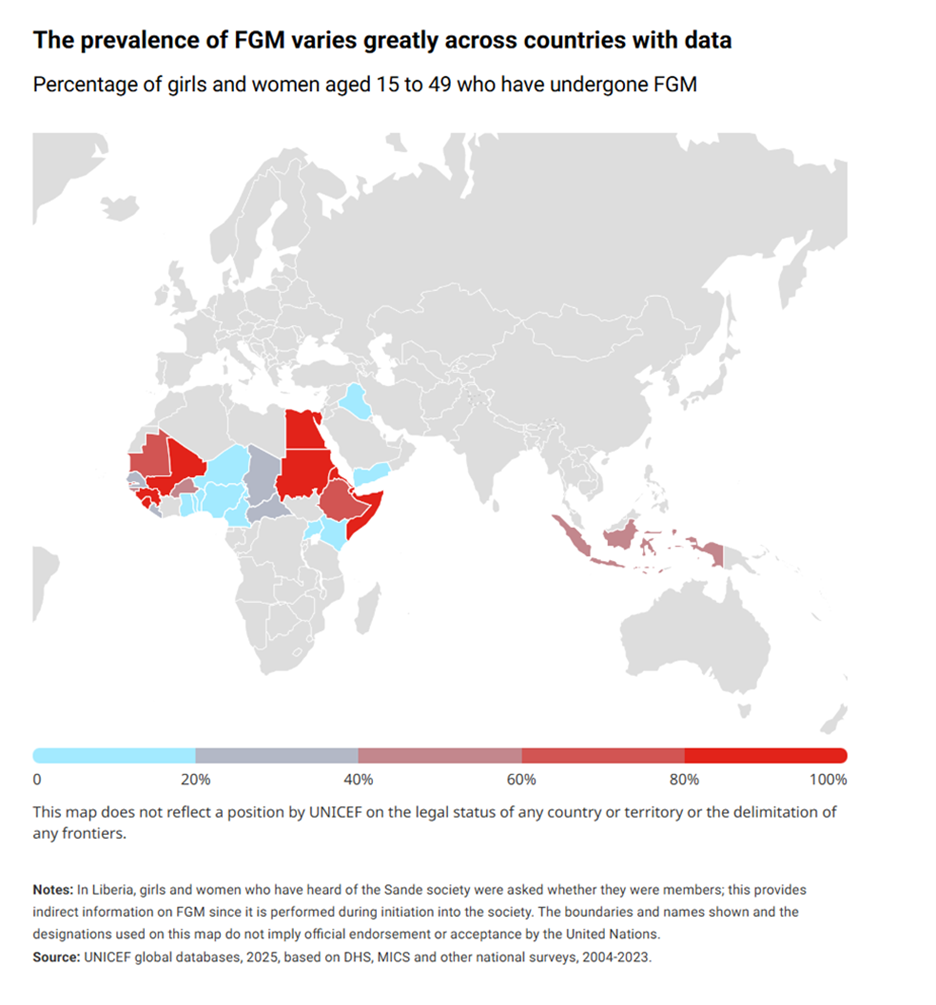
Prevalence in newcomer populations in Canada
The prevalence of FGM/C in newcomer populations is difficult to gauge, and Canadian data are lacking. However, the Ontario Human Rights Commission has identified evidence to indicate that FGM/C is practiced in Canada.[5] A 2025 study by Islamic Relief Canada reported both that FGM/C is performed in Canada, and that girls are taken overseas to have it done.
In some communities, parental intentions regarding FGM/C for their daughters decline following immigration. However, the factors influencing their change in outlook are not fully understood. Health care providers should be aware that even in countries with a high prevalence of FGM/C, there are high levels of opposition to the practice. UNICEF reports that 400 million people in African and Middle Eastern countries where FGM/C is practiced say they want it to end.[1]
Myths and misconceptions
There are numerous myths and misconceptions concerning FGM/C, including that the practice[3]:
- Is supported or mandated by religion
- Is an important cultural tradition that should not be questioned or stopped, particularly not by outsiders
- Prepares a girl for adulthood and marriage
- Reduces a women’s sexual desire, preserves virginity and prevents promiscuity
- Improves male sexual pleasure and virility
- Facilitates childbirth by increasing a women’s pain tolerance
- Facilitates cleanliness
- Prevents the clitoris from growing excessively
Risk Factors
Risk factors for FGM/C are summarized in Table 1.
|
Table 1: Risk factors for FGM/C |
|
|
Age |
FGM/C is typically performed at some point between infancy and age 15 years. In half the 29 countries where FGM/C is most commonly practiced, >80% of cutting occurs in girls <5 years of age. |
|
Region |
Prevalence varies greatly among countries and there is also substantial variation within countries. Countries where the prevalence of FGM/C is highest (>80%) include Somalia, Guinea, Djibouti, Egypt, Eritrea, Mali, Sierra Leone and Sudan. Data on prevalence by country is detailed in Figure 1. |
|
Religion |
The prevalence of FGM/C is highest among Muslim girls and women, but this is not always the case. FGM/C is also reported among individuals from other religious backgrounds. |
|
Urban vs. rural |
FGM/C prevalence tends to be lower in wealthy urban residents, perhaps because they have exposure to a greater number of socio-cultural networks. |
|
Economic status |
The prevalence of FGM/C is generally lower in relatively wealthier households. |
|
Education level of mother |
The prevalence of FGM/C is generally highest among daughters of women with no education. |
|
FGM/C in mother |
The chances that a girl will undergo FGM/C are significantly increased if her mother has been cut. |
|
Sources: Adapted from references 2, and 3. |
|
Types of FGM/C
The WHO identifies 4 types of FGM/C, which are summarized in Table 2 and illustrated in Figure 2.[2]
|
Table 2. Types of FGM/C[2] |
|
|
1 |
Partial or total removal of the clitoris and/or the prepuce (clitoridectomy). |
|
2 |
Partial or total removal of the clitoris and labia minora, with or without excision of the labia majora (excision). |
|
3 |
Narrowing of the vaginal orifice with creation of a covering seal by cutting and appositioning the labia minora and/or the labia majora, with or without excision of the clitoris (infibulation). Adhesion of the labia results in near complete covering of the urethra and vaginal orifice, which must be reopened for sexual intercourse and childbirth (defibulation). |
|
4 |
All other harmful procedures to the female genitalia for nonmedical purposes (e.g., pricking, piercing, incising, scraping, cauterization). Pricking or nicking involves cutting to draw blood, with no removal of tissue or permanent alteration of the external genitalia, sometimes referred to as symbolic circumcision. |
Figure 2. Types of female genital cutting (FGC)

|
A, Tissue removed in type 1 FGC: partial or total removal of the clitoris and/or the prepuce (clitoridectomy). B, Appearance after type 1 FGC. C, Tissue removed in type 2 FGC: partial or total removal of the clitoris and the labia minora, with or without excision of the labia majora (excision). D, Appearance after type 2 FGC. E, Tissue removed in type 3 FGC: narrowing of the vaginal orifice with creation of a covering seal by cutting and appositioning the labia minora and/or the labia majora, with or without excision of the clitoris (infibulation). F, Appearance after type 3 FGC. Illustrations reproduced with permission from the artist, Jessica Stanton, MD. © 2013 Mayo Foundation for Medical Education and Research |
|
Source: Adapted with permission from reference 4. In Somalia, most women who underwent FGM/C had their genitalia sewn closed.[7] |
Complications
FGM/C is recognized as harmful to girls and women, both physically and psychologically, and has no medical benefit.[4] The occurrence of trauma and medical complications may relate to[3][4]:
- The type of FGM/C
- The type of practitioner
- The absence or misuse of anesthesia
- The type of equipment used (scissors, razor blades, and/or broken glass may be used)
FGM/C is widely performed by traditional practitioners, but health practitioners do perform the procedure in some regions of the world, and their involvement appears to be increasing.[2] In Egypt, an estimated 77% of procedures are carried out by a doctor, nurse, midwife or other health worker, and nearly always with an anaesthetic being used. By contrast, an estimated 97% of cases in Yemen underwent the procedure in their homes, and 75% of these girls were cut using a blade or razor. No information is available regarding the use of an anesthetic in these settings.[8]
Early complications
Early complications are usually treated by a local practitioner, and patients may only present to a health care professional for complications that are significant or occur well after the procedure.[3] Early complications include severe pain, bleeding, infection and urinary retention and are associated more frequently with FGM/C types 2 and 3, as shown above.[3]
Later complications
Later complications of FGM/C are summarized in Table 3.[3]
Evidence of the effect of FGM/C on fertility is mixed,[3] but it can be affected long term by a number of factors, such as the physical barrier created by certain types of FGM/C, scarring or stenosis, and infections of the uterus or adnexa. FGM/C may be associated with psychological issues, such as dyspareunia and fear of sexual encounters, affective disorders, anxiety, post-traumatic stress disorder and somatization.[3] No randomized trials of the impact of FGM/C on pregnancy outcomes have been carried out to date.[9]
|
Table 3. Later complications of FGM/C[4] |
|
|
Type of complication |
Strongly associated with FGM/C (in case reports and/or cohort studies) |
|
Fertility/sexuality |
Anorgasmia, apareunia, decreased satisfaction, dyspareunia, lack of sexual desire, vaginal dryness |
|
Infection |
Bacterial vaginosis, herpes simplex virus |
|
Pain |
Clitoral neuroma, dysmenorrhea; lower abdominal, vaginal or vulvar pain |
|
Psychological |
Anxiety, depression, post-traumatic stress disorder, somatization |
|
Scarring |
Fibrosis, hematocolpos, keloids, labial fusion (partial or complete), sebaceous cysts, vaginal stenosis, vulvar abscesses |
|
Urinary |
Chronic urinary tract infections, meatal obstruction, meatitis, urethral stricture, urinary crystals |
|
Source: Hearst AA, Molnar AM. Female genital cutting: An evidence-based approach to clinical management for the primary care physician. Mayo Clin Proc 2013;88(6):618-29. Adapted with permission. |
|
What health practitioners can do
Health care providers who see newcomer girls and adolescents in their practice should be aware of FGM/C and be ready to provide culturally sensitive, clinically informed care, including early recognition and management of the complications. Patients may present with an early complication of FGM/C, but in Canada they are more likely to present with later problems.[3] A health provider should treat such cases as per standard practice, but may also need to make appropriate investigations and enlist specialist support. Clinicians can play a key role to ensure that women who have undergone this procedure receive proper care and support by:
- Informing themselves about this practice, asking questions, and gauging the level of support and perspectives on FGM/C in families they see.
- Being open to discussing this issue with patients and families.
- Providing counselling and support or appropriate referrals for girls/adolescents and their parents, as needed. The Society of Obstetricians and Gynaecologists of Canada (SOGC) notes that adequate and respectful counselling or support might entail involving a culturally competent interpreter or social worker.[5]
- Revisiting the issue. Not all patients or families will be open to counselling on such a personal topic at the first clinical encounter. Raising the issue again, once a relationship of trust is established, is likely to be more effective.
- Offering physical examination of genitalia as part of screening.
- Performing physical examination in a sensitive manner, when consent is obtained, to identify presence and type of FGM/C and any complications (particularly infection, labial fusion/vaginal stenosis and keloids or other evidence of scarring). Guidance for genital examination of paediatric patients is available in this Pediatrics in Review article.[10]
- Recognizing and treating complications.
- Prevention. Questions to consider asking a newcomer patient (from regions where FGM/C is practiced) or her family are listed below.[11] A sensitive introduction is important. Consider some version of this approach: ‘I would like to discuss a very personal aspect of your daughter’s health with you – called circumcision or cutting – Do you mind if we speak about this?’ ‘Is circumcision a common practice in your country? In your family? Are you comfortable sharing your thoughts and feelings about this practice?’
Possible questions to consider
- Family (maternal) history: Have the women in your family (your mother or grandmother) been circumcised? If so, please share your experience. Where was it done? By whom? What was your age at circumcision? How do women in your family feel about circumcision?
- Community/context: Do you talk about circumcision with other women? Your daughters? Do you know anyone who is not circumcised? What have you heard?
- Beliefs: What do you think is good about being circumcised? What are the troublesome aspects of being circumcised? Does your religion recommend circumcision? Is circumcision for women normal in your culture or family?
- Plans/concerns: How would you feel about your daughters not being circumcised in Canada? How do you think your daughter would feel if she is not circumcised? How do you think your daughter’s future husband would feel if your daughter is not circumcised?
- Difficult scenarios: Do you hope to be able to circumcise your daughter? In Canada, circumcision is not legal, how does that affect your plans? Are you aware of the laws relating to circumcision in Canada?
For patients who have already experienced FGM/C
Discussing FGM/C with girls/adolescents and their parents can be challenging. Still, studies generally show that most women who have had FGM/C would like their physician to discuss the topic with them in a proactive way: that is, when it pertains to a current or anticipated health or family problem.[3] Possible questions can include:
- Do you (or your daughter) have any pain/discomfort/problems because of this procedure? Are there any other problems or feelings you would like to share? And especially: What medical help would you like for any of these problems?
“When the physician (rather than the patient) initiates the questions in a way that is normalized as part of the woman’s [overall] health history, it can help to overcome the patient’s or the interpreter’s embarrassment about the topic.”[4]
Selected resources
- Sauer PJ, Neubauer D. Female genital mutilation: a hidden epidemic (statement from the European Academy of Paediatrics). Eur J Pediatr 2014; 173: 237-238.
- UNICEF FGC page
- UNICEF resource: Female Genital Mutilation/Cutting country profiles
- United Nations General Assembly. 67/146. Intensifying global efforts for the elimination of female genital mutilation: Report of the Secretary-General (2024)
- WHO. Female genital mutilation
References
- UNICEF. Female genital mutilation. 2024 Mar.
- World Health Organization. Female genital mutilation: key facts. 2025 Jan.
- United Nations Population Fund (UNFPA). Female genital mutilation (FGM): frequently asked questions. 2025 Feb.
- Hearst AA, Molnar AM. Female genital cutting: an evidence-based approach to clinical management for the primary care physician. Mayo Clin Proc. 2013;88(6):618–29.
- Ontario Human Rights Commission. FGM in Canada. [date unknown].
- Perron L, Senikas V, Burnett M, et al. Female genital cutting. J Obstet Gynaecol Can. 2013;35(11): 1028–45.
- FGM/C Research Initiative. Somalia. 2021.
- Yoder PS, Wang S, Johansen E. Estimates of female genital mutilation/cutting in 27 African countries and Yemen. Stud Fam Plann. 2013; 44(2):189–204.
- Balogun OO, Hirayama F, Wariki WM, Koyanagi A, Mori R. Interventions for improving outcomes for pregnant women who have experienced genital cutting. Cochrane Database Syst Rev. 2013;2:CD009872.
- Jacobs A, Alderman E. Gynecologic examination of the prepubertal girl. Pediatr Rev. 2014;35(3):97–105.
- Upvall MJ, Mohammed K, Dodge PD. Perspectives of Somali Bantu refugee women living with circumcision in the United States: a focus group approach. Int J Nurs Stud. 2009;46(3):360–8.
Reviewer(s)
Brittany Anne Howson-Jan, MD
Andrea Hunter, MD
Last updated: February, 2026
